
| Connect & Subscribe |
How I Survived Maxillo-Mandibular Advancement (MMA) Surgery
Getting your jaw cut off and bolted back on is about as fun as it sounds. That's basically what's involved in maxillo-mandibular advancement (MMA), but it's the most effective surgery for sleep apnea and could save your life. It looks like this:
I underwent MMA surgery about a year and half ago, and even though recovery sucks, if you have moderate or severe apnea you should definitely think about getting it done.
Before I had surgery, I talked to a couple of people who had undergone MMA. Every one of them said it was absolutely worth doing and had been tremendously beneficial for them. Now that I've been through it, I would absolutely recommend it for anyone with moderate or severe sleep apnea. Hearing about their MMA experiences from them helped me make my decision to go through with it, so I've written about my experience here in hopes that it'll be helpful to anyone who is considering surgery.
Diagnosis
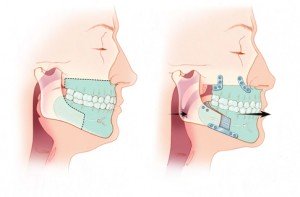 Image from SleepApneaSurgery.com
Image from SleepApneaSurgery.com
I had chronic fatigue growing up, and at age 19, a doctor finally ordered a sleep study for me at the Stanford Sleep Medecine Center. I was diagnosed with sleep apnea with a respiratory disturbance index of 30, meaning that I would wake up 30 times per hour while sleeping. This put me on the borderline between "moderate" and "severe" apnea. My dad also had symptoms of chronic drowsyness, and he got diagnosed around the same as I did. His apnea was even worse, with a respiratory disturbance index of over 150.
In both my case and my dad's, our apnea was caused mostly by a receding jaw, which made us both good candidates for MMA surgery. I was an especially good candidate, because young people recover from surgery more readily and because young people are notoriously non-compliant with CPAP.
Surgery: Round One
Before undergoing MMA, many surgeons will recommend having more minor surgeries to clear out the airway without breaking the jaw. My first round of surgeries was performed by Dr. Winston Vaughan at Stanford Hospital and included a tonsillectomy, bilateral nasal turbinate reduction, septoplasty, concha bullosa resection, and adenoidectomy. He also trimmed my soft palate and uvula. The surgery was performed under general anaesthesia.
I expected this first round of surgery to be relatively minor, since it was just soft tissue being removed. As it turned out, the tonsillectomy was vastly more painful than the MMA turned out to be. My surgeon warned me that the tonsillectomy would be painful, but I was not at all prepared for how painful it was.
You can find lots of advice on how to survive a tonsillectomy if you look online, but the two things I would emphasize are ice water and vicodin. Some people have problems with nausea when taking vicodin, but if you can stomache it, it's a fantastic painkiller. Also, tonsillectomies are far more painful for adults than children, so if you have a child with sleep apnea (or if you are one), get a tonsillectomy sooner rather than later.
At the recommendation of my jaw surgeon, I also got my wisdom teeth removed. He recommended having it done at least 9 months before the MMA surgery, but I had it done only 6 months before the MMA and it worked out fine.Surgery: Round Two
My MMA surgery was performed by Dr. Kasey Li at Stanford Hospital. His website is SleepApneaSurgery.com, and according to other doctors I spoke to, he's supposed to be one of the best surgeons in the world at performing MMA. He's supposedly performed over a thousand of them.
The surgery took 5 hours, which I'm told is pretty typical. Dr. Li advanced my jaw by 12 millimeters. My dad had had the same surgery about a month before I did, and he had his jaw advanced 20 millimeters. Looking at my X-rays, I count 6 titanium plates and 28 screws holding my jaw together.
I wasn't in much pain when I woke up from the anaesthesia, but my face was numb and incredibly swollen. I don't have any pictures, unfortunately, but "chipmunk" does not even begin to describe it. You have no idea how swollen your face can get until you've tried MMA surgery. Also, at some point I realized I was catheterized, which was disconcerting but very understandable in hindsight.
I spent two nights in the hospital before being discharged, which is also pretty typical for MMA.
My health insurance covered most of the cost. I believe that in total, it cost $108,000, but I only had to pay a few thousand out of pocket.
Recovery
Here's a few things that were helpful when I was recovering:
- Vicodin. The pain got worse after I was discharged from the hospital, but it never got anywhere near as bad as the tonsillectomy. That's good news, in a way -- if you can get through a tonsillectomy, MMA surgery really isn't so bad. I took vicodin for the first week or so after being discharged, but I was fine without painkillers after that. My dad, interestingly, didn't need painkillers at all.
- A small whiteboard, or an iPad or other tablet. For the first four weeks after surgery, the patient's mouth is rubber-banded shut, which makes it pretty hard to talk. The rubber bands are attached to "arch bars", which are kind of like dental braces except that they're anchored by wires between the teeth instead of being cemented onto the teeth. The rubber bands started out tight enough that I couldn't talk at all, but after two weeks I had periodic follow-ups with Dr. Li in which he replaced the rubber bands with looser ones that let me talk a bit. During those first two weeks, I carried around either a small whiteboard or an iPad with a text-to-speech app so I could communicate.
- Gallons of apple juice. It's hard to eat with your jaw rubber-banded shut. You're going to lose a lot of weight -- I lost around 10 pounds before my weight stablized. It's very helpful to have some kind of liquid to drink that also has some calories. I ended up drinking loads of apple juice, but some other fruit juice would probably have worked just as well.
- A blender. Getting enough calories with your jaw wired shut is tough. After some trial and error, I ended up finding a meal I could prepare easily that had enough calories to get me by: A tin of sardines and a hunk of goat cheese blended into potato-and-leek soup. I know -- that sounds disgusting -- but it was actually not half bad. I've heard that "hunger is the best spice", and it's true. It tasted great to me at the time, and it packed a lot of calories. My weight was dropping until I discovered this recipe, but it stabilized after that.
- A Waterpik Flosser. You're not going to be able to brush your teeth with your jaw rubber-banded shut, but it's good to be able to clean out stuff from your puree'd meals that gets caught in your teeth. The Waterpik is a little device squirts a stream of water at your teeth, which lets you clean the outside of them pretty well. Since you can't brush, this is the next best thing for making your mouth feel clean.
I had the surgery during Christmas break, and I went back to school after two weeks. If you're thinking about surgery, I would recommend a bare minimum of two weeks off before returning to school or work. I think how much time off you need depends largely on your age when you have the surgery. My dad, who was 50 at the time, needed a full month off of work.
My jaw was still rubber-banded shut when I went back to school, but I could talk enough to get by. My face was also still fairly swollen, though nowhere near as bad as it had been. It took several months for the swelling to go all the way down.
My chin and palate were numb following the surgery. It took about a month for feeling to return to my chin and about six months for it to return to my palate.
Results
The surgery has been tremendously beneficial for me. I feel much more alert during the day. During high school, I used to fall asleep in class reliably every day, whereas now I feel pretty well-rested most days. I haven't been back for another sleep study, mostly because even if I still have some apnea, there isn't anything left I could do about it (except CPAP, which I couldn't tolerate.)
But even if it hadn't helped my sleep apnea, it would have been worth it for the cosmetic improvement alone. I inherited my dad's receding jaw, which is not an attractive feature, and even 12mm more jaw was a dramatic improvement. I've spoken with several other people who had the same procedure, and all of them were very happy with both the improvement to their sleep and to their appearance.
So if you're thinking about getting MMA surgery for sleep apnea, go for it. It's totally worth it.
And join the conversation with your own comments here:
blog comments powered by DisqusAbout This Site
Welcome! This site is continuously being created by students of Dr. William C. Dement's Sleep And Dreams course at Stanford University.
We made this site as a call to action for people all over the world to live healthier, happier, safer, and more productive lives by learning about their own sleep. We have faith that reading the information provided on this site will motivate you to be smart about your sleep deprivation and strategic about your alertness in order to live life to your fullest, most energetic potential.
In fact, we challenge you to do so! What do you say, are you up for the challenge?
Interviews With Sleep Specialists: Insights Into the Worlds of Sleep Medicine & Sleep Business
America's Most Dangerous Disorder: What Is Sleep Apnea Doing To Your Sleep?
Sleep Debt: How Much More Will You Achieve When You Reduce Yours?
The Stages Of Sleep: The Journey Through The Night
Delayed Sleep Phase: You Want To Sleep But You're Not Tired Yet
Paralyzed at Night: Is Sleep Paralysis Normal?
Sleep In Words: Smart, Strange, and Funny Quotes About Sleep
Sleep Disorders In Children: What's Keeping Your Child From A Full Night's Rest?
Attacks of Pavor Nocturnus (a.k.a. Sleep Terrors, Night Terrors, or Incubus Attacks)
The Stanford Sleep Book
Dr. Dement's pioneering textbook has been the core text for Sleep and Dreams since 1980, but it has just recently been made available to the wider public for the first time.
In it you'll find a more detailed account of the most important things you need to know about sleep, alertness, dreams, and sleep disorders. Studies, statistics, plus plenty of Dr. Dement's classic anecdotes painting the history of sleep medicine.
Preface | Intro | Contents | Get A Copy
More Sleep Resources
The Zeo
A revolution in personal sleep tracking, the Zeo is a wireless headband that transmits your brainwaves in realtime to a dock (pictured here) or your smartphone. The result? You can wake up and see exactly what stages of sleep you were in during the night! Unprecedented personalized sleep knowledge.
Sleep Paralysis: A Dreamer's Guide
Ever woken up paralyzed? A surprising number of us have, believe it or not. But few know the actual causes of this phenomenon, and fewer still how to exert control over it. Dream researcher and sleep paralysis expert Ryan Hurd shares breakthrough insights into how to do just that.
Important Disclaimer
Please Note:
The information found on this page and throughout this site is intended for general information purposes only. While it may prove useful and empowering, it is NOT intended as a substitute for the expertise and judgments of healthcare practitioners.
For more info, see our
Terms of Use.









